A Baker’s Cyst is a fairly common condition that is also known by the more technical term, popliteal cyst.
Many people are surprised to learn that knee injuries, arthritis, gout, or other issues can be the cause of the fluid-filled sacs in the back of the knee referred to as a Baker’s cyst.
Having a better understanding of how this condition develops and the associated symptoms can prevent them from happening in the first place, or at least from becoming worse.
Learning about the best options for Baker’s cyst treatment and early intervention techniques can be effective ways to decrease injury-related downtime.
What is a Popliteal or Baker’s Cyst?
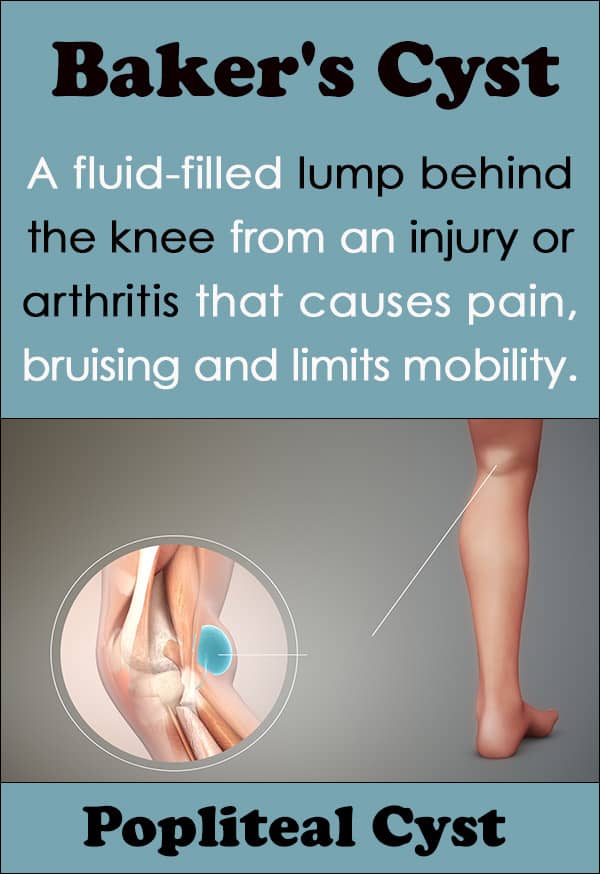
A Baker’s cyst is a soft, fluid-filled lump at the back of the knee that is named for the physician that first described it, in this case Dr. William Morrant Baker in the mid-1800s.
It is sometimes referred to as a Popliteal Cyst because they occur in the popliteal fossa, which is an area behind the knee containing nerves, veins, and arteries.
A Baker’s cyst behind the knee develops because an injured knee produces extra synovial fluid, a clear liquid that runs through the cavities of the knee-joint to decrease friction between the cartilage and joint. The excess fluid can only flow in one direction, which increases pressure, inflammation, and swelling, and leads to a synovial-filled bulge.
While the cysts may be painless in some cases, others experience moderate to severe pain, as well as a limited range of motion because of swelling, inflammation, and discomfort with knee extension.
These types of popliteal cysts may go away on their own, but if left untreated, they can also worsen. From time to time, a Baker’s cyst ruptures, sending fluid down the inside of the calf and presenting as a bruise.
Blood clots can also lead to bruising and swelling at the back of the knee and calf. Clots can be a serious health concern, which is why it’s important to see a physician at the first sign of a lump or discomfort in this area of the body.
What are Typical Causes of a Baker’s Cyst?
Unfortunately, knees are complex joints and can be easily injured or damaged. While athletes are typically the focus of discussion with most knee injuries, non-athletes are certainly not exempt from this condition.
Aging knee-joints with a lot of wear and tear or arthritis are at high risk of injury, as well as knees supporting an unhealthy amount of bodyweight.
The Most Common Baker’s Cyst Causes Include:
- A torn or ruptured meniscus, the cartilage inside the knee
- Osteoarthritis in the knee
- Rheumatoid arthritis in the knee
- Ligament tears in knee
- Inflammation from other conditions, such as gout
Whatever the cause of a popliteal cyst, the symptoms can be uncomfortable and downright painful.
Baker’s Cyst Symptoms
Some people with a Baker’s cyst behind the knee will feel little to no pain and might not even be aware that they have a cyst. In others, however, the pain from a popliteal cyst can be significant and lead to other problems.
Baker’s Cyst Symptoms May Include Some of the Following:
- Mild to severe pain at the back of the knee, sometimes radiating down the calf
- Inflammation, swelling, or a bulge at the back of the knee and calf
- Stiffness or limited range of motion
- Bruising at the back of the knee and calf
- A burst or rupture of the synovial fluid
Treatment approaches for Baker’s cysts generally start with conservative options and then, depending on severity, move forward with more invasive methods.
What are Effective Baker’s Cyst Treatment Methods?
It’s important to have a Baker’s cyst diagnosed by a physician, in order to rule out a more serious health issue like a blood clot.
Proper diagnosis will require a physical exam, a discussion about a person’s medical history, and possibly x-rays, an MRI, or ultrasound so a physician can have a clear image of the knee and any associated damage.
A doctor will want to know when the symptoms first appeared, what activities trigger the pain, and if it is persistent or comes and goes, among other things.
It’s possible that a small or discreet Baker’s cyst will go away on its own, although a large one that causes pain should be treated to avoid getting bigger or rupturing.
7 Ways to Treat a Baker’s Cyst
If symptoms persist and the popliteal cyst becomes larger or more painful, the following treatment options can be helpful.
1. RICE Method
The RICE Method involves Rest, Ice, Compression, and Elevation. Resting the injury at the first signs and applying an ice pack to the area can be effective for reducing pain and inflammation, allowing the cyst to heal and go away on its own.
Rest can range from limiting painful activities to using crutches to alleviate any pressure on the area.
In addition, a compression bandage around the knee will limit movement and elevating the knee above the heart while resting can help with healing.
2. Anti-Inflammatory Pain Medication
Over-the-counter, nonsteroidal anti-inflammatory pain medication, like ibuprofen (Advil) or naproxen (Aleve) is also useful for pain and swelling. Using these while resting the knee can help reduce inflammation.
3. Physical Therapy
Physical therapy, sometimes in combination with EPAT therapy, is helpful for strengthening the knee, and learning proper form or techniques to prevent further injury or damage.
Some forms of physical therapy can teach patients about gentle exercises and stretches they can then do on their own to maintain knee strength and flexibility.
4. EPAT Therapy (Shockwave)
EPAT Therapy stands for Extracorporeal Pulse Activation Technology, and it is a noninvasive treatment approach that delivers impulse pressure waves deep into the back of the knee. EPAT can increase blood flow, decrease swelling, and help break up the cyst.
EPAT Therapy is also known as Extracorporeal Shockwave Therapy or ESWT, and it is an effective method for treating and healing pain for a wide range of conditions related to sports injuries or aging.
Two to three EPAT treatments about a week apart generally result in a favorable outcome that speeds up the healing process. The more energy a patient can tolerate, the quicker the cyst can be broken up.
5. Steroid Injections
Steroid injections for extremely inflamed knee joints may be recommended, but this powerful anti-inflammatory can damage other, healthy tissue.
Some sports physicians suggest that younger to middle aged patients avoid steroid injections if possible because of the long-term damage they can have on otherwise healthy patients.
6. Draining the Baker’s Cyst Synovial Fluid
Sometimes draining the synovial fluid from the knee and cyst is necessary by inserting a needle and directing it to the proper area with the aid of ultrasound.
It’s important to find the root cause of the fluid buildup to treat the underlying condition as well. If the knee experiences an injury such as a torn ligament, that injury will also need to be repaired so the knee heals properly.
If the initial injury is not corrected, the fluid might build up again and could cause the Baker’s cyst to re-appear. When this happens it will need to be drained again.
7. Surgery
Surgery, which will come with a significant recovery downtime, is usually a last resort and limited to the most extreme cases. Arthroscopic surgery, called scoping, can be used to both diagnose and repair damaged tissue.
A knee osteotomy is a procedure used by surgeons to cut a portion of bone to correct any structural damage to the knee. There are always associated risks with surgery and these procedures should be thoroughly discussed and considered beforehand.
For anyone who is concerned that pain and swelling behind the knee might be a Baker’s cyst, they should make an appointment to get it examined by a doctor as soon as possible.
In the meantime, some of the treatment methods outlined here should be a good place to start before receiving a proper diagnosis. Resting the knee will help with healing and over-the-counter medications can reduce pain and inflammation.
Bake’s Cyst image courtesy of Scientific Animations.